Neonatal syphilis remains a serious but preventable condition that affects newborns exposed to syphilis during pregnancy. Without early intervention, congenital syphilis can lead to severe complications, long-term disability, or even death. Effective management of newborns born to mothers with syphilis is therefore critical in safeguarding the child’s health and future.
Understanding the Goal of Management
The primary aim in managing a newborn exposed to syphilis is to prevent and treat congenital syphilis early. This approach significantly reduces the risk of complications and ensures better outcomes for the infant.
Management is guided by several important factors:
The mother’s treatment history
The stage of maternal infection
Clinical findings in the newborn
Laboratory test results
1. Maternal Assessment
The first and most crucial step is evaluating the mother’s medical history. Healthcare providers must determine:
Whether the mother received treatment
If the treatment was adequate (correct penicillin regimen completed at least four weeks before delivery)
Maternal RPR/VDRL titres
Possibility of reinfection during pregnancy
An untreated or inadequately treated mother significantly increases the baby’s risk of infection.
2. Clinical Examination of the Newborn
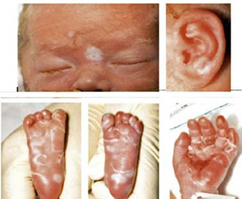
A thorough physical examination of the baby is essential. Signs of congenital syphilis may include:
Enlarged liver and spleen (hepatosplenomegaly)
Skin rash or peeling
Persistent nasal discharge (“snuffles”)
Jaundice
Anemia
Bone tenderness or reduced limb movement (pseudoparalysis)
Poor feeding
Any presence of these signs should prompt immediate treatment for congenital syphilis.
3. Investigations in the Baby
Laboratory tests help confirm diagnosis and guide treatment decisions. These may include:
Baby’s RPR/VDRL test (compared with maternal titres)
Full Blood Count (FBC)
Cerebrospinal fluid (CSF) analysis for VDRL, protein, and cell count (if infection is suspected)
X-ray of long bones
Liver function tests (LFTs)
4. Treatment: The Most Critical Step
Treatment depends on both maternal history and the baby’s condition.
A. If the Mother Was Not Treated or Inadequately Treated
The baby should receive a full course of penicillin:
Aqueous Crystalline Penicillin G
50,000 IU/kg per dose intravenously
Every 12 hours (first 7 days of life)
Every 8 hours (after 7 days)
For a total of 10 days
OR
Procaine Penicillin G
50,000 IU/kg intramuscularly once daily for 10 days
B. If the Mother Was Adequately Treated and the Baby is Well
If the newborn shows no symptoms and has low antibody titres:
Benzathine Penicillin G
50,000 IU/kg intramuscularly as a single dose
C. If Congenital Syphilis is Proven or Highly Suspected
The baby must receive a full 10-day course of intravenous or intramuscular penicillin, regardless of maternal history.
5. Follow-Up Care
Ongoing monitoring is essential to ensure treatment success:
Repeat RPR/VDRL testing at 3, 6, and 12 months
Antibody titres should gradually decrease over time
If titres do not decline appropriately, retreatment is necessary
6. When to Strongly Suspect Congenital Syphilis
Certain situations should raise immediate concern:
High maternal antibody titres
Lack of antenatal care or treatment
Premature or small-for-gestational-age baby
History of stillbirth
Presence of hydrops fetalis
7. Potential Complications if Untreated
Failure to treat congenital syphilis can lead to devastating outcomes, including:
Hearing loss (deafness)
Vision problems or blindness
Bone deformities
Developmental delays
Death
Conclusion
Neonatal syphilis is preventable, treatable, and manageable when identified early. Proper maternal screening during pregnancy, timely treatment, and careful newborn assessment are the pillars of prevention.
Every healthcare provider and caregiver plays a vital role in ensuring that no child suffers from a disease that can be effectively controlled. Early action is not just medical care—it is a life-saving intervention.
Understanding the Goal of Management
The primary aim in managing a newborn exposed to syphilis is to prevent and treat congenital syphilis early. This approach significantly reduces the risk of complications and ensures better outcomes for the infant.
Management is guided by several important factors:
The mother’s treatment history
The stage of maternal infection
Clinical findings in the newborn
Laboratory test results
1. Maternal Assessment
The first and most crucial step is evaluating the mother’s medical history. Healthcare providers must determine:
Whether the mother received treatment
If the treatment was adequate (correct penicillin regimen completed at least four weeks before delivery)
Maternal RPR/VDRL titres
Possibility of reinfection during pregnancy
An untreated or inadequately treated mother significantly increases the baby’s risk of infection.
2. Clinical Examination of the Newborn
A thorough physical examination of the baby is essential. Signs of congenital syphilis may include:
Enlarged liver and spleen (hepatosplenomegaly)
Skin rash or peeling
Persistent nasal discharge (“snuffles”)
Jaundice
Anemia
Bone tenderness or reduced limb movement (pseudoparalysis)
Poor feeding
Any presence of these signs should prompt immediate treatment for congenital syphilis.
3. Investigations in the Baby
Laboratory tests help confirm diagnosis and guide treatment decisions. These may include:
Baby’s RPR/VDRL test (compared with maternal titres)
Full Blood Count (FBC)
Cerebrospinal fluid (CSF) analysis for VDRL, protein, and cell count (if infection is suspected)
X-ray of long bones
Liver function tests (LFTs)
4. Treatment: The Most Critical Step
Treatment depends on both maternal history and the baby’s condition.
A. If the Mother Was Not Treated or Inadequately Treated
The baby should receive a full course of penicillin:
Aqueous Crystalline Penicillin G
50,000 IU/kg per dose intravenously
Every 12 hours (first 7 days of life)
Every 8 hours (after 7 days)
For a total of 10 days
OR
Procaine Penicillin G
50,000 IU/kg intramuscularly once daily for 10 days
B. If the Mother Was Adequately Treated and the Baby is Well
If the newborn shows no symptoms and has low antibody titres:
Benzathine Penicillin G
50,000 IU/kg intramuscularly as a single dose
C. If Congenital Syphilis is Proven or Highly Suspected
The baby must receive a full 10-day course of intravenous or intramuscular penicillin, regardless of maternal history.
5. Follow-Up Care
Ongoing monitoring is essential to ensure treatment success:
Repeat RPR/VDRL testing at 3, 6, and 12 months
Antibody titres should gradually decrease over time
If titres do not decline appropriately, retreatment is necessary
6. When to Strongly Suspect Congenital Syphilis
Certain situations should raise immediate concern:
High maternal antibody titres
Lack of antenatal care or treatment
Premature or small-for-gestational-age baby
History of stillbirth
Presence of hydrops fetalis
7. Potential Complications if Untreated
Failure to treat congenital syphilis can lead to devastating outcomes, including:
Hearing loss (deafness)
Vision problems or blindness
Bone deformities
Developmental delays
Death
Conclusion
Neonatal syphilis is preventable, treatable, and manageable when identified early. Proper maternal screening during pregnancy, timely treatment, and careful newborn assessment are the pillars of prevention.
Every healthcare provider and caregiver plays a vital role in ensuring that no child suffers from a disease that can be effectively controlled. Early action is not just medical care—it is a life-saving intervention.